Site-neutral payments could lead to $7.4 billion in Medicare cuts
Legislation with the site-neutral proposal that researchers found would provide the most federal savings was recently introduced in the Senate.
A study of previously proposed Medicare site-neutral payment policies found overall they would have cut the targeted payments by 50% across affected services.
The findings come as Congress reportedly considers implementing various forms of site-neutral payment policies in Medicare to reduce federal spending.
The study, published in June in Health Affairs, found three previous site-neutral policy proposals would cut federal Medicare $212 million to $7.4 billion, annually.
“Given the way we modeled the saving, that was within the magnitude we expected,” Kathryn Linehan, associate scientist at the Center for Health Systems and Policy Modeling at Johns Hopkins University, said about the federal savings the proposals would have generated.
The magnitude of the federal savings across the three proposed site-neutral policy changes was driven by:
- Number of ambulatory payment classifications (APCs) targeted
- Total spending on those APCs
- Scope of application (off-campus hospital outpatient departments only or all hospital outpatient departments)
- Policy alignment of outpatient prospective payment system (OPPS)service payments with either Medicare physician fee schedule or ambulatory surgical center rates
The study “arrayed the way those different levers affected any savings/budgetary impact” of site-neutral proposals, Linehan said.
Why it matters
The research comes as Congress considers a massive budget reconciliation package that includes tax cuts and nearly $800 billion in reduced increases in Medicaid spending over 10 years. Some members of Congress have urged the addition of site-neutral payments in Medicare to provide more federal savings to that package.
For example, Sen. Rick Scott (R-Fla.) recently urged lawmakers to align Medicare payments for services in hospital outpatient departments with the lower payments for similar services in independent physician offices.
In 2023, Congress advanced legislation. the Lower Costs, More Transparency Act (HR5378), through the House to equalize Medicare Part B payments for drug administration across settings — one of the proposals studied in the new research. Previous proposals would have applied to even broader segments of Medicare-covered services.
In early 2025, House Republicans offered a list of cuts to consider that included “site neutrality” payments estimated to save $146 billion over a decade. Those were not included in the House-passed budget reconciliation package now before the Senate.
In May, Sen. John Kennedy (R-La.) introduced legislation with site-neutral payments previously proposed by the Medicare Payment Advisory Commission (MedPAC) — another of the three proposals studied by the new research.
Proposals reviewed
The new research examined the various financial effects of three previous site-neutral proposals:
- HR5378, which would limit site-neutral payments to four drug administration APC codes at off-campus sites
- A 2024 analysis of the Actuarial Research Corporation (ARC) of 12 APC codes (including drug administration, imaging and diagnostic services) at off-campus hospital outpatient departments only
- A 2023 recommendation from MedPAC, which applied to 66 APC codes at both on- and off-campus sites
A goal of the research was to provide a standardized comparison of the three proposals, which previously had projected financial effects by separate and differing types of estimates.
The researchers found HR5378 would generate the least federal one-year savings ($212 million) and the ARC option would have saved $516 million in 2021. Meanwhile, the MedPAC option yielded the highest potential one-year savings, $7.4 billion. The research may undercount overall federal savings, Linehan said, because it did not account for such implications as the effect of lower rates on Medicare Advantage payments.
The analysis found, in aggregate, the 66 APCs identified by MedPAC were performed in physician offices 65.9% of the time.
Effects by hospital type
Most of the federal savings from the three proposals would come from payment cuts to hospitals with:
- Larger numbers of beds
- Nonprofit ownership
- Teaching status
- Metropolitan location
“Basically, the budgetary savings are in proportion to OPPS revenue,” Linehan said.
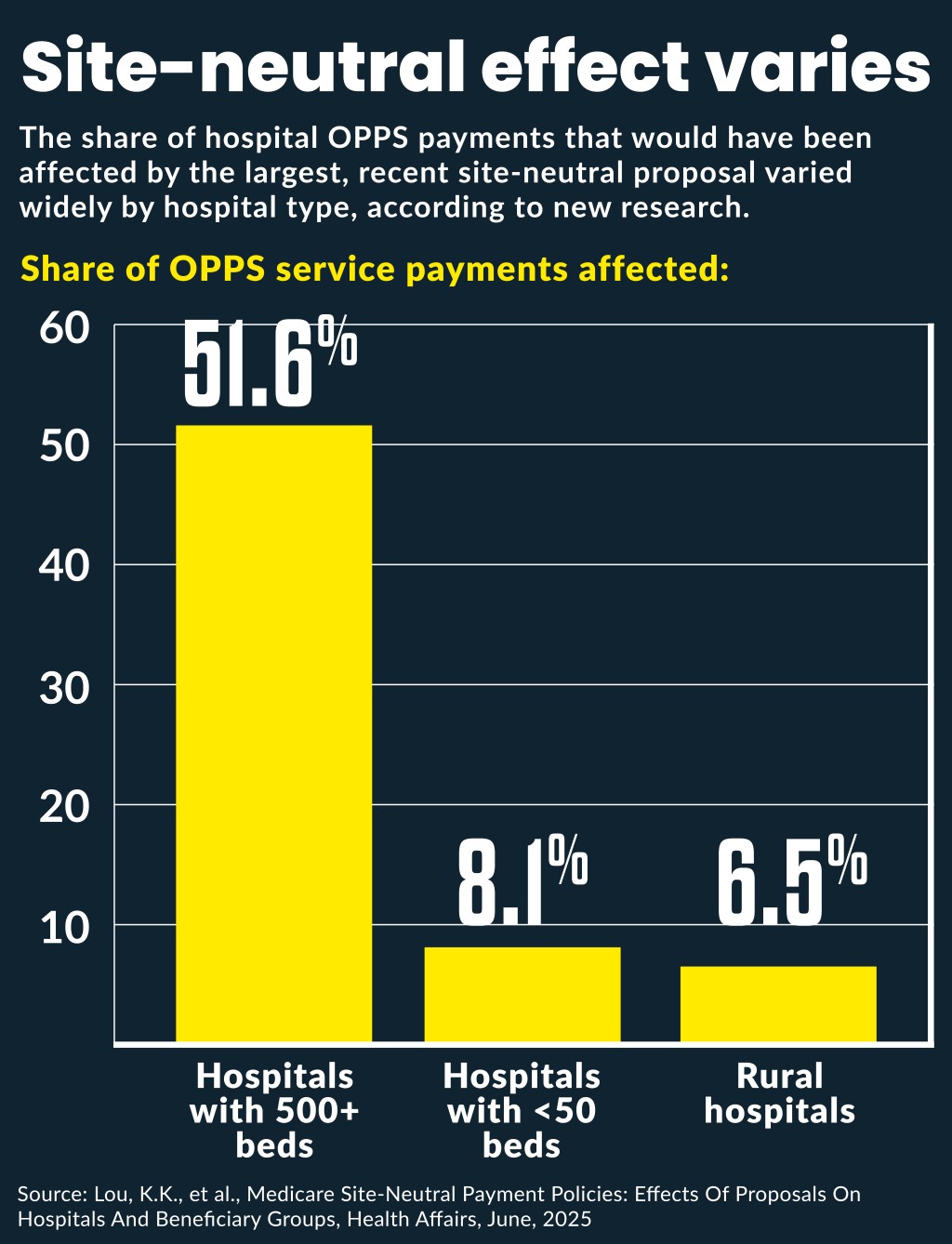
The site neutral policies would affect 28.2% to 51.6% of total OPPS service payments to hospitals with more than 500 beds, which received 28.7% of all OPPS service payments in 2021, the researchers found.
Meanwhile, only 4% to 8.1% of the proposals’ generated savings would come from OPPS payments to hospitals with fewer than 50 beds, which received 6.2% of all OPPS service payments in 2021. The study found that rural hospitals received 5.1% of all OPPS service payments in 2021 and the cuts would affect from 2.7% to 6.5% of their OPPS payments.
The finding on rural hospitals followed HR5378 stalling in the Senate over concerns about its adverse financial effect on rural hospitals.
“Our finding shows small and rural hospitals paid under Medicare’s OPPS system would absorb the smallest shares of the proposed cuts,” said Linehan. “But, as we point out, we don’t assess what share of their revenues that is. So that could vary.”
Under the most aggressive site-neutral option (from MedPAC), $6.2 million of the $7.4 billion generated one-year savings would come from metropolitan hospitals.
The projected impacts on teaching hospitals come as NIH grant terminations by the Trump administration have pulled almost $2 billion in funding away from U.S. medical schools and hospitals, according to a new analysis from the Association of American Medical Colleges.
The latest site-neutral proposals also come as hospital margins have stagnated in 2025, based on the latest Strata Decision Technology data. The median year-to-date operating margin for health systems dipped to 0.9% in March from 1% in both January and February, marking the first time since 2023 that the metric was below 1%.





