Rhode Island’s hospital price limits linked to 9.1% cut in hospital prices over 10 years
The effects of the state's cost-control program were especially large in the fully insured market, which is subject to state regulation.
A unique rate-limiting program in Rhode Island was linked to a 9.1% cut in hospital prices over 10 years, much of which was passed along to commercially insured plans and enrollees, according to recent research.
The findings (subscription required), recently published in Health Affairs, could bolster a program that has been under siege in recent years as some hospitals in the state struggle financially.
“Hospital prices in Rhode Island are still some of the lowest in the country, so it’s quite clear that the [price limiting regulatory] standards played an important role in containing hospital price growth, notwithstanding some recent increases,” said Andrew Ryan, a professor at Brown University, and an author of the study.
The price-limiting program was launched in 2010 by the state’s health insurance commissioner using authority under state law. The initiative capped increases in hospital negotiated rates with fully insured commercial plans, first, to annual CMS Medicare hospital payment updates, plus 1%. Beginning in 2016, hospital rate increases were limited to the Consumer Price Index plus 1%. The commissioner’s office also limited premium increases for the fully insured (about 30% of commercial coverage by the end of the study period). Self-insured commercial plans are only regulated under federal law.
Study results
The 2012 to 2022 effects of the state’s approach, according to the study, included:
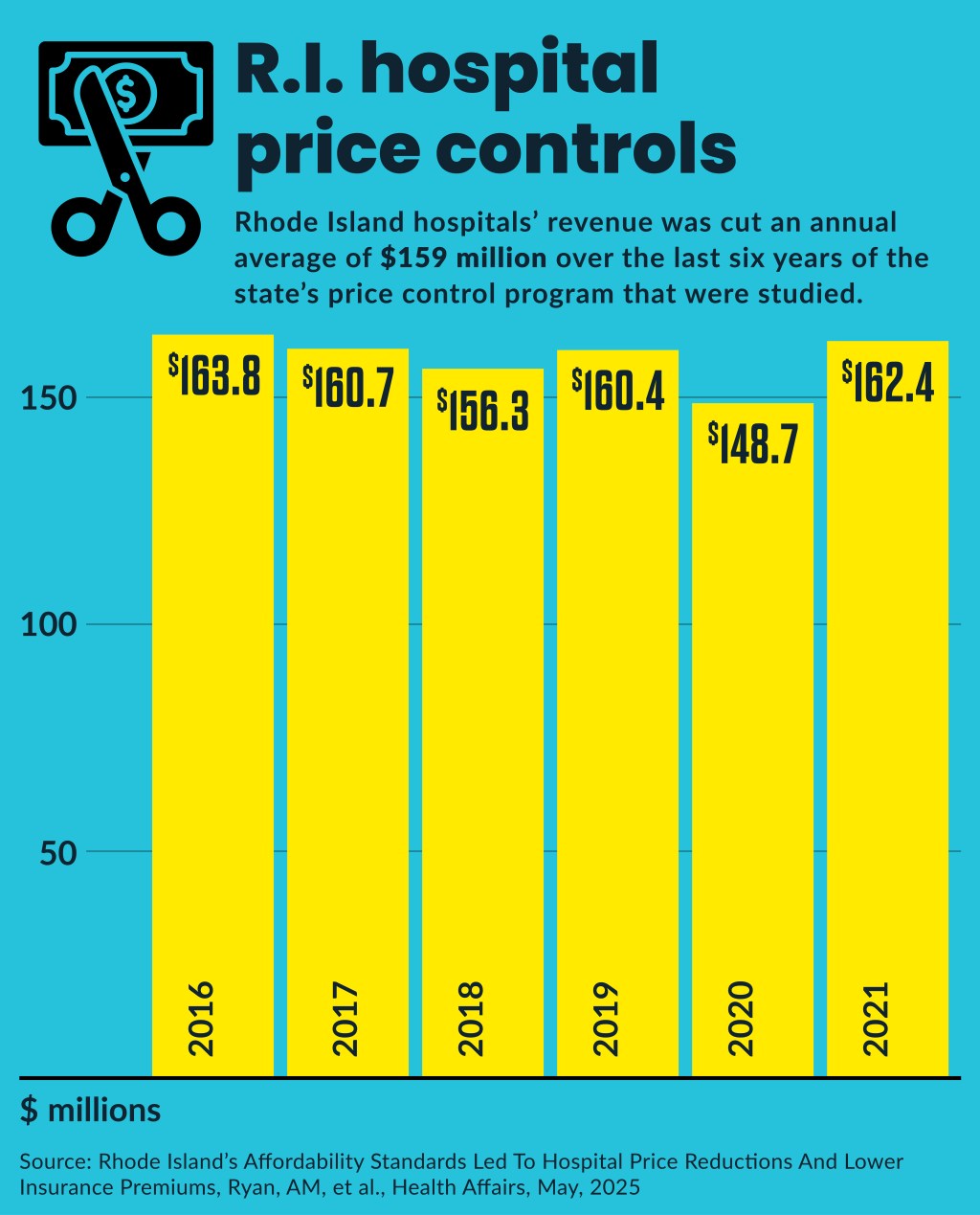
- $158.3 million average annual cut in aggregate hospital commercial plan revenue
- Average 9.1% cut in hospital prices relative to comparison states in both fully insured and self-insured plans
- Commercial plan hospital prices decreased from 106% of the national average to 84% of the national average
- Fully insured premiums decreased from an average of $1,200 more expensive than in comparison states to $219 more costly
- Average annual $449 (6.5%) relative reduction in fully insured premiums
- $206 (2.7%) relative increase in annual single premiums for large employers (likely self-insured)
- $96 (5.5%) increase in deductibles for the entire commercial market
Although the study did not track the size of the hospital revenue cut by year, Ryan said it strongly increased over the years of the study and would likely be more than $158 million in the years after 2022.
“It’s really more recent years where these effects really started to intensify, where those price differences manifested,” Ryan said.
The study was the first to examine the effect of state cost-control strategies on both premiums and hospital finances.
Also noteworthy: The pass-through effects of restricted hospital prices on payer premiums were not limited to the fully insured plans that states could regulate but also occurred to a lesser extent in self-insured plans.
“That really surprised us, but it was confirmed to us when talking to people that insurers just negotiate a single fee schedule across segments; they don’t use different prices for different segments,” Ryan said.
Hospital effects
Rhode Island hospital operating margins averaged −0.4% after the initiative launched, according to hospital cost reports, and that compared to 4.8% operating margins, nationally. The study did not track annual changes in the margin over the policy period.
“I think the Rhode Island hospital margins have been worse in more recent years,” Ryan said.
Some of that deterioration could have come from unrelated trends and policy changes in recent years, including a steady decrease in commercial plans’ share of the state’s payer mix and Medicaid cuts during the study period. That likely resulted in lower recent hospitals margins than the average found over the study period, he said.
The study found operating margins for Rhode Island hospitals were concentrated around 0.00%, while those for hospitals in comparison states were more dispersed.
Based on a definition from the National Academy for State Health Policy Hospital Cost Tool, they found Rhode Island hospital operating margins averaged 14%, compared to a 17.2% average, nationally.
“This suggests that hospital operating margins were lower in Rhode Island than in comparison states after the” policy was implemented, the authors wrote.
R.I. policy outlook
Ryan said the state’s cost control policy is “somewhat controversial” and legislation was introduced last year to repeal it amid concerns it was harming hospitals’ finances. However, the governor has defended it as helping to improve healthcare affordability.
“You have some disputes among hospitals and the administration as to what is happening here and what is the value of these standards,” Ryan said.
However, he said, hospitals were not uniformly opposed to the cost control measures.
The Rhode Island Hospital Association did not respond to a request for comment on the study or the cost control program.
National ramifications
The findings on the Rhode Island cost control initiative may inform hospital price control initiatives in other states.
In early May, Indiana enacted a law that could revoke the nonprofit status of larger health systems if their aggregate inpatient and outpatient charges exceed the state average.
The Washington state legislature also recently passed legislation to cap rates paid to hospitals for services delivered to various state government employees. The bill would cut payments to hospitals across the state by an estimated $170 million annually when fully implemented.
Various hospital price control bills have been proposed in North Carolina, Vermont, Nevada and Colorado.
“States are kind of getting fed up. They have been trying various strategies, like transparency, and they’re starting to take more aggressive action,” Ryan said.





