More rural hospitals adopt critical access status to boost finances
The change reflects a reassessment by some larger rural hospitals of the long-held assumption that increases in admissions eventually will turn around their finances.
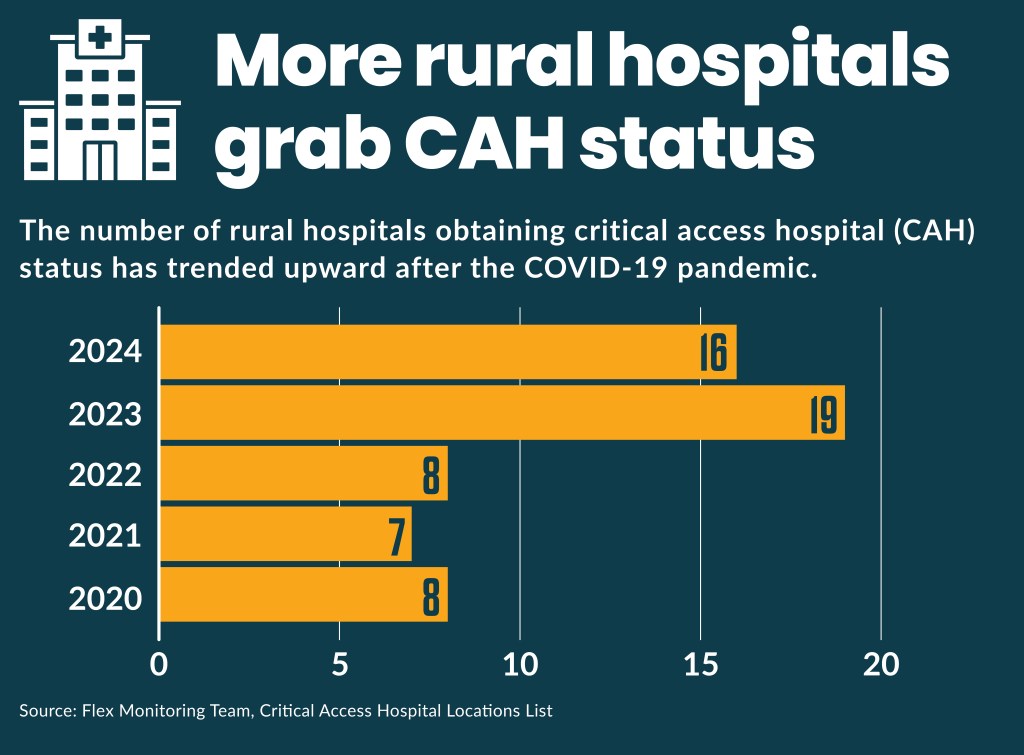
More rural hospitals are agreeing to reduce their inpatient beds by switching to critical access hospital (CAH) status, which many subsequently used to obtain 340B eligibility.
The increase in hospitals obtaining CAH status and 340B eligibility comes amid an ongoing trend of closures and service line eliminations as rural facilities financially struggle. Those adverse consequences stem, at least partly, from changing rural patient preferences.
“The patients will bypass their local hospitals to get services that their local hospital could do with some quality,” John Gale, senior research associate, Maine Rural Health Research Center at the University of Southern Maine. “They see those bigger hospitals as being better and that’s not always true.”
Sixteen rural hospitals obtaining CAH in 2024 and 19 did so in 2023, compared to 8 obtaining it in 2019, before the COVID-19 pandemic, according to a tracking site.
Nine of the hospitals obtaining CAH status in 2024 have, so far, subsequently become eligible for the 340B discount drug program. Medicare disproportionate share hospitals (DSH) must have an adjustment percentage greater than 11.75% to qualify for 340B but there is no adjustment percentage requirement for CAHs. CAHs had nearly $1 billion in 340B purchases in 2023, according to the Health Resources and Services Administration.
It was a path pursued by Wayne Hospital, a 32-licensed-bed hospital in Greenville, Ohio. The hospital recently converted to CAH status, which capped it at operating 25 beds. However, a Fitch Ratings report noted its average patient census was only nine over the past five years.
The status change to CAH increased its Medicare payment rates to 101% of reasonable costs and was credited by Fitch as the driver of “markedly improved fiscal operations” in FY24. The ratings agency changed the hospital’s outlook from stable to positive based on the resulting financial improvements.
“Conversion to a CAH allowed [Wayne Hospital] to begin receiving cost-based reimbursement from Medicare in 3Q 2024,” said the Fitch report. “On a full-year basis, this should provide for a $15 million to $25 million increase to annual revenues compared to FY 2023 levels with the same patient volumes.”
Fitch noted the $15 million revenue increase the hospital obtained from only six months of CAH status was “well above” estimates of the hospital’s leaders.
Additionally, Wayne Hospital executives told Fitch they were “exploring the potential for new revenues” from the 340B program and planned to apply for entry in July 2025.
Broader struggle
Rural hospitals have financially struggled for many years. In 2023, operating margins were lower among hospitals in rural areas (3.1%) than hospitals in urban areas (5.4%), according to a KFF report. And operating margins were worse (1.7%) among the nearly 1,000 hospitals in rural areas that either do not include and are not closely connected to any substantial population center.
Since 2010, 182 rural hospitals “closed or converted to an operating model that excludes inpatient care,” according to recent Chartis report. That analysis concluded that 46% of rural hospitals are operating at a loss, and 432 are vulnerable to closure.
One factor hurting hospitals’ ability to maintain inpatient staffed beds is rural patients bypassing those facilities. For example, a 2023 study of 121,297 rural elective surgery visits found 65% bypassed their local hospital.
“There was a period where the bigger [rural] hospitals were resistant [to reducing beds through CAH conversion] because they thought the larger number of beds was their ticket to success,” Gale said. “As the contribution of the inpatient services change, CAH becomes a little more attractive.”
However, conversion to CAH status has not always been enough to prevent closures of rural hospitals. Since 2010, 51 CAH have closed, compared to only slightly more closures (59) among prospective payment hospitals (PPS) hospitals, according to tracking by the Sheps Center at UNC.
Despite their challenges, the outlook of CAHs executives has improved in recent years. Ninety-six percent of executives with rural healthcare organizations — primarily CAHs — were optimistic about their organization’s financial viability, according to an ongoing survey from Wipfli. That share was an increase from 84% in 2023 and 91% in 2024.
Other options
Beyond conversion to CAH status, the range of options for rural hospitals to stabilize their finances has changed in recent years.
Converting to REH. For instance, 32 rural hospitals have converted to rural emergency hospitals (REHs) since that option launched in January 2023. That option directs CAHs and other small hospitals to drop inpatient services for emergency department and other outpatient services. In exchange, they receive more than $3 million in annual facility payments and a 5% increase for all services covered under the Medicare OPPS.
About 400 facilities are “most likely” to consider REH, with 77 identified as prime candidates for the new designation, according to a Chartis analysis.
Joining a health system. Another traditional option for financially struggling rural hospitals has been acquisition by a health system. A recent study of 202 CAHs that joined a hospital system between 2011 and 2021 found they had a mean 1.3% increase in total margin.
However, recent tracking of hospital deals has found the financially distressed organizations targeted by health systems for acquisition are no longer mainly small, rural hospitals.
Forming a network. A growing number of rural hospitals are forming a network with other rural hospitals in their state to improve their outlook by collaborating on clinical and business initiatives. Recently the Ohio High Value Network was formed among 25 rural hospitals in that state. It followed the 2023 launch of the Rough Rider High-Value Network in North Dakota and the 2024 creation of the Headwaters High-Value Network in Minnesota.






