For-profit health systems turn to AI and automation to manage payer denials
Surveys show major continuing challenges in hospitals efforts to leverage AI in the revenue cycle, as payers have already done.
Despite challenges with the technology, some for-profit health systems are increasingly looking to AI and other automation tools to tackle the worsening problem of payer denial management.
Seventy-three percent of providers have seen claims denials increase, according to a 2024 survey by Experian Health. That included 38% saying denials occur on at least 10% of claims and 11% who had denials on 15% of claims.
Despite the increasing challenge from denials, nearly half of respondents were still manually reviewing claims and fewer were using AI or some form of automation technology (31% in 2024 versus 62% in the same survey in 2022).
Leaders’ views
But some health systems are eyeing such technologies to provide a revenue cycle boost and potentially labor cost savings.
“AI adoption in claims denial management is emerging, rather than widespread,” said Rajiv Sheth, a partner at Guidehouse. “Leading health systems are exploring AI to counter payer denials, often using agentic AI alongside human staff for optimal results. This allows organizations to prioritize the biggest opportunities to address.”
Kevin Hammons, CFO for Community Health Systems, said his organization is both developing its own AI tools and purchasing some from vendors.
“There’s some AI use cases in the revenue cycle with denial management, so forth,” Hammons said at a March 18 investor conference. “It’s going to be very important. It’s kind of a force multiplier if you will, and we’re certainly looking to make some investments.”
Steve Filton, CFO for Universal Health Services said at the same March 18 conference that his organization is moving toward using more of the technology.
“What AI can do if used properly is help you predict what claims are likely to draw greater scrutiny to help you ensure you have done all of the things to make the claims are as clean and problem free as possible,” Filton said. “We do that now in a manual way and there’s potential for that to be more automated and for AI to help do that. And we’ve made some improvements in that regard but we will continue to do so.”
Similarly, HCA Healthcare is investing in AI, machine learning and robotic process automation (RPA) in many areas including revenue cycle, Mike Marks, CFO of HCA, said at a March 20 investors’ conference.
Ardent Health Services credits its EHR and revenue cycle vendor for the last two and half years for helping it drive down denials, which Marty Bonick, CEO of the 30-acute hospital system described as a “big issue across the industry.”
“It’s still a big issue but because of technology, we’ve invested in and they’ve invested in, we believe we are doing better than average to deal with those challenges and pressures that we have,” Bonick said at a March 19 investors’ conference.
Sheth said AI adoption is more prevalent in well-funded, advanced health systems and markets where payers aim to narrow profit margins with providers. Meanwhile, rural hospitals and independent systems show lower adoption rates.
Technology dissatisfaction
AI automation adoption faces a range of obstacles, according to industry consultants. Those can include: an initial high cost of deploying AI solutions; a need for high-quality, standardized data to deliver accurate insights; and staff hesitancy to adopt AI-driven workflows due to concerns about job displacement or unfamiliarity with the technology.
Despite a range of technological approaches used by health systems to both understand and address claims denials, there was broad dissatisfaction with the tools used, according to an HFMA survey sponsored by FinThrive.
Findings on technology used for claims denial analytics included:
- 48% using an EHR alone
- 37% using a vendor embedded in their EHR
- 27% using a vendor not embedded in their EHR
But the overall assessment of the health systems’ technologies used for claims denial analytics was extreme in nature.
- 29% were highly satisfied
- 39% were highly dissatisfied
Health systems took a similarly diverse approach to denials management technologies:
- 60% using EHR capabilities only
- 16% using a vendor embedded in their EHR
- 19% using a vendor not embedded in their EHR
But both satisfaction and dissatisfaction with denials management technologies selected by health systems also was high:
- 37% were highly satisfied
- 33% were highly dissatisfied
Sheth said the ROI timeline for AI in RCM varies widely based on implementation, data quality, and specific use cases. Early adopters report seeing initial improvements within six to 12 months, with more significant returns realized over two to three years as AI models mature and integrate fully.
Need increasing
Despite health systems’ challenges with denials management technology, more may pursue the time and labor cost savings they can provide because the cost of denials continues to increase.
“Hospitals need AI to level the playing field as payers increasingly leverage AI for claims reviews and denials,” Sheth said. “AI can help hospitals manage the growing data volume and staffing shortages, preventing margin erosion.”
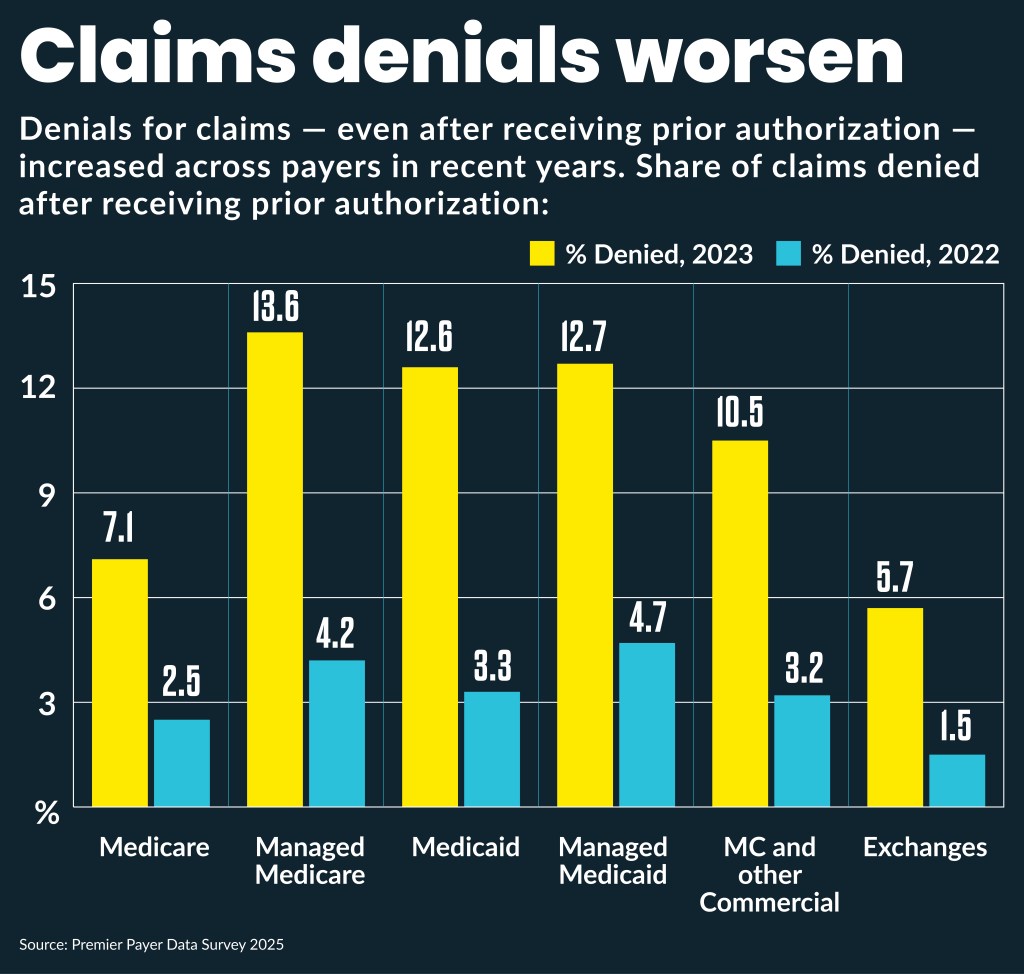
A newly released survey and analysis of member hospitals by Premier found claims adjudication cost healthcare providers more than $25.7 billion in 2023, or 30% more than the $19.7 billion identified in 2022.
Additionally, it found the administrative costs associated with fighting claims denials increased dramatically, from $43.84 per claim in 2022 to $57.23 in 2023. The additional costs primarily resulted from added labor, responsible for 90%of claims processing expenses incurred by providers.
Premier also reported that 70% of disputed denials are overturned and paid.
“This means that nearly $18 billion was potentially wasted arguing over claims that should have been paid at the time of submission,” said a Premier press release.





