Idaho is fourth state to require financial data from 340B entities
Five other states have active 340B reporting bills in the current legislative session.
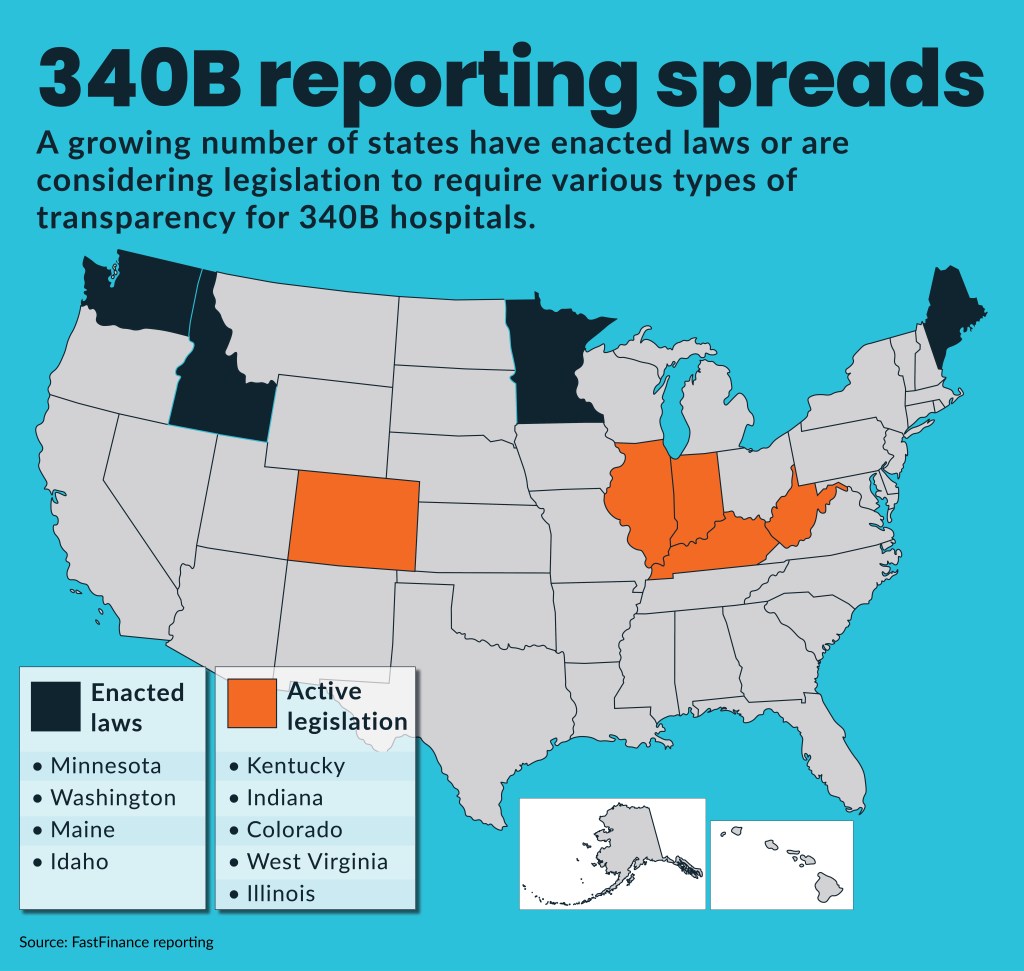
Recently enacted Idaho legislation will require 340B covered entities to report a range of financial information to the state.
The state joins three others with 340B covered entity (CE) reporting laws and five other states considering similar requirements in the current legislative session.
The Idaho law, signed April 1 by Gov. Brad Little (R), requires CEs to report 340B-related data to the Department of Health and Welfare, the state controller and the attorney general every April.
The CE data required by HB 136 includes:
- Aggregate acquisition cost for 340B drugs
- Aggregate payment amount received for 340B drugs
- Aggregate payment made to 340B contract pharmacies
- How 340B CEs used 340B savings (including charity care and community benefits)
“It’s just one more piece of legislation that adds a regulatory burden at a time when ensuring hospitals are viable in their communities is really difficult,” said Toni Lawson, vice president of external relation for the Idaho Hospital Association (IHA).
More than half the state’s 51 hospitals have less than a 1% margin, she said.
The bill arose suddenly after the sponsor of a separate bill to protect 340B contract pharmacies decided more information was needed before that measure could advance and introduced HB 136, said Lawson.
The bill’s unclear language also has raised questions for hospitals on some requirements and which elements will be publicly reported, she said.
Idaho’s new reporting law followed similar measures enacted in recent years by Minnesota, Maine and Washington.
Sometimes intermingled with 340B reporting requirements are legislative initiatives in more than 30 states to block drugmaker restrictions on the use of 340B contract pharmacies. Nine states, including Delaware and Missouri, have enacted such contract pharmacy protection legislation into law.
Indiana advances bill
The five states that continue to consider 340B reporting legislation include Indiana, where the House passed a 340B transparency bill April 1.
CE reporting in Indiana’s SB 118 includes many elements also in the Idaho law but also would add:
- Aggregate payments made to any other entity that is not a contract pharmacy
- Aggregate payment made for any other 340B administering expense
- Number and percentage of low-income patients of the CE served using a sliding fee scale for 340B drugs
- Copies of 340B CEs’ financial assistance policies for the reporting year
Hospital advocates have raised concerns that the Indiana bill creates undue administrative burden for safety-net providers that rely on 340B to expand access to care.
The Indiana Hospital Association (IHA) “looks forward to continuing conversations with state legislators to ensure the final bill meets the original intent for greater transparency without adding to the cost of health care for Hoosier hospitals and their patients,” Scott Tittle, president of IHA, said in a written statement.
The measure has been sent back the Senate, which previously passed it, with amendments to exclude 340B grantees and add $1,000-per-day fines for late reporting.
Colorado
The Colorado Senate passed a bill on March 26 with similar 340B reporting requirements as the Indiana and Idaho bills delineated by payer type, including commercial, Medicaid and uninsured.
However, the Senate amended the bill to strip out language requiring CEs to use 340B revenue to decrease out-of-pocket costs for low-income patients, as well as adding language to bar drug manufacturer access restrictions for sole community hospitals and critical access hospitals.
The bill has moved to the House for consideration.
The Colorado Hospital Association has criticized the bill as a giveaway to drugmakers and for imposing burdensome reporting requirements on health care providers.
Kentucky
A bill (HB 685) in Kentucky would require nonprofit hospitals to submit a 340B Drug Pricing Program report to the Cabinet for Health and Family Services every July. It also would require state reports on the impact of the 340B program on both the Kentucky Employee Health Plan and Medicaid.
The reporting requirements for 340B hospitals echo those of other state legislation but also require reporting on total payments to third-party administrators for managing any aspect of the CE’s 340B program and the number of contract pharmacies located outside Kentucky as well as the location of those pharmacies.
Another different reporting requirement included “a detailed and itemized accounting of expenditures associated with 340B profits, including an itemized report of all programs, services, equipment purchases, staffing, and any other expenditures financed, in part or in whole, by 340B profits.”
The legislation has not advanced since its introduction.
West Virginia
West Virginia bill SB 675, introduced in March, echoes many of the reporting components of other state transparency bills, including how 340B revenue is used for charity care, community benefits, “or a similar program of providing unreimbursed health care to the indigent.”
It also would require that the information be broken down by payer type but would not publicly release the data.
The bill directs the West Virginia Board of Pharmacy to aggregate and report the data and analyze “how the covered entity uses any savings from participating in the 340B program including how the savings are used for the provision of charity care, community benefits, or a similar program of providing unreimbursed health care to the indigent.” That report would be publicly posted.
The bill has not advanced.
Illinois
The Illinois legislature introduced HR 158 in February. The bill would direct the auditor general to conduct a comprehensive investigation of “the amount of 340B profit, defined as total patient and payer reimbursement less the total 340B acquisition cost, generated by 340B covered entities from both self-administered and physician-administered drugs,” among other provisions.
Other areas it would investigate include:
- Amount spent on third party administrators to manage the 340B program
- Amount going to pharmacy benefit managers (PBM) in contract pharmacy arrangements
- Amount going to contract pharmacies
- Average CE “mark-up” on 340B drugs
- Extent to which 340B CEs pass 340B discounts to vulnerable patients at the point of sale
HR 158 has not yet advanced.






