Potential government changes are top concern for healthcare finance professionals
Forty-two percent of respondents said their organization will need to remove more than 5% of their costs over the next three years to remain financially sustainable.
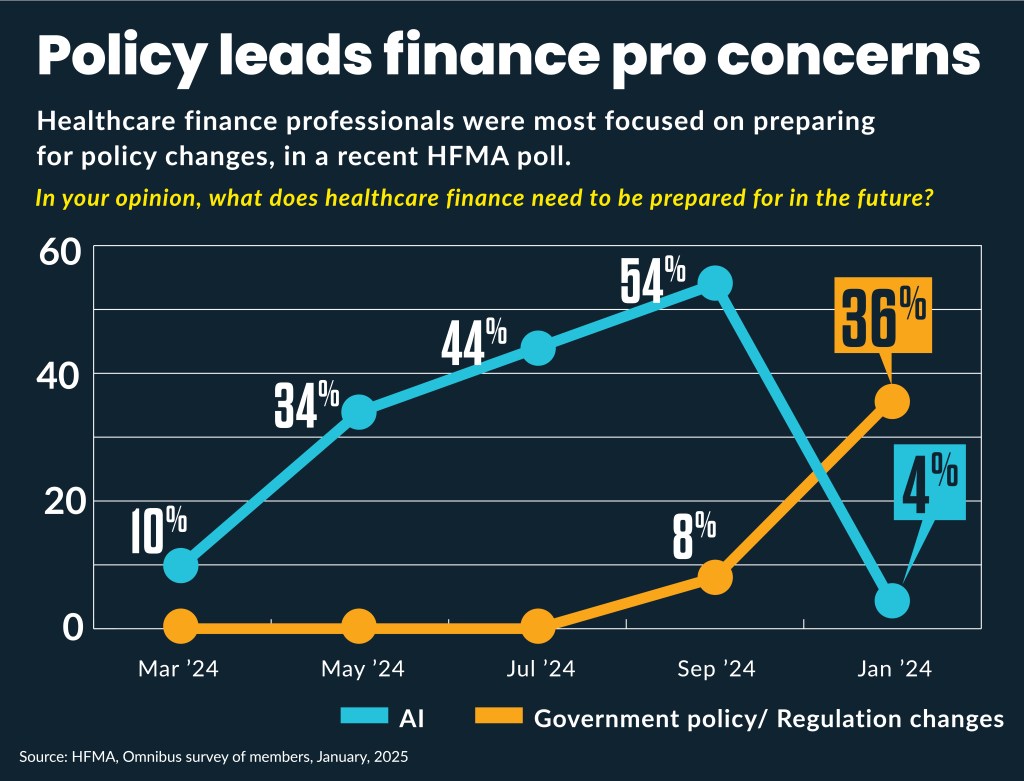
Potential government and regulatory changes jumped to the leading concern of healthcare finance professionals, according to latest HFMA member poll.
Thirty-six percent of the respondents in the December poll of one-twelfth of HFMA members named policy changes as the leading area requiring preparation, which was a big increase from the 8% who identified it as the leading issue in the previous poll in November. The second-highest area where planning was needed, according to the latest poll was 24% who identified payer and insurance challenges.
The results come amid a range of initiatives by the Trump administration and the Republican-led Congress to cut federal spending on healthcare.
The Trump administration implemented a 15% cap on indirect costs for NIH grants, a policy which is facing a series of legal challenges. It also has sent members of the Department of Government Efficiency (DOGE) to review the payment systems of the CMS.
Additionally, congressional Republicans have advanced a budget that would cut as much as $880 billion from the projected $1.6 trillion increase in Medicaid spending over the next 10 years.
“You take away Medicaid and you end up with bed debt and charity or sicker patients because they are delaying care,” said Kimberly Hodgkinson, former CFO of Hospital Sisters Health System. “I’m not sure [policymakers] always think about the ins and outs of decisions.”
Transparency push
Among policy changes expected from the administration is a doubling down on price transparency requirements for hospitals that started in Trump’s first administration. In a Feb. 25 executive order (EO), President Donald Trump noted that his first administration drafted the two sets of regulations requiring providers and insurers to make prices available to healthcare purchasers.
He thinks the Biden administration put insufficient emphasis on the regulations after starting to implement them in 2021, even though enforcement increased in recent years and the templates for hospitals to use in publishing their machine-readable files became more exacting.
The EO “directs the Departments of Treasury, Labor and Health and Human Services to rapidly implement and enforce the Trump healthcare price transparency regulations, which were slow-walked by the prior administration,” according to a White House statement.
For their part, HFMA survey respondents saw the biggest effect of the expanding transparency requirements in improving their organization’s ability to secure premium rates for specialized services that they provide. Smaller positive effects were seen in either improving their competitiveness in their market or helping them negotiate with a payer.
Revolutionizing healthcare finance
HFMA members’ concern about federal policy changes may not mean they expect those changes to either last or have major effects. That’s because only 6% thought policy changes would be the next big thing to revolutionize healthcare finance.
Instead, such revolutionary change in healthcare finance was expected to come from either AI and automation (28%) or revenue cycle and billing (24%).
But the industry’s fervor on the promise of AI appeared to cool in the latest results. Only 4% of respondents said AI was the leading area in which they needed to prepare. That was down from 54% who prioritized AI preparation in the November survey.
Similarly, the share of organizations that planned to invest in AI in the coming 12 to 18 months dipped to 38%, down from 41% with such plans in a September poll of HFMA members.
The top investment priority for respondents’ organizations remained “facilities design, construction and management,” which was the case for much of the past year.
However, extending the expected investment outlook to three years led most (58%) of respondents to name health information technology as likely to require the most spending.
The only category of employment on which respondents expected their organization to increase spending within the next three months was on fully employed clinicians. Meanwhile, hiring of contract clinicians, full-time administrative staff or contract administrative staff was expected to remain flat or decrease.
Cost cutting
A substantial share of respondents (42%) said their organization will need to remove more than 5% of their costs over the next three years to remain financially sustainable. That compared to 47% who thought they would need to cut 1% to 5% of costs and 11% who did not see a need to remove any costs.
Labor cost/productivity was expected to provide cost savings opportunities among 41% of respondents. While fewer saw savings opportunities in service line efficiency (35%) or supply chain and non-labor costs (33%).
The leading impediment respondents identified to their organization’s ability to achieve cost savings was a lack of leadership accountability in such efforts (20%). Smaller shares blamed a lack of data and insight on where to find savings (13%) or the political sensitivity of savings opportunities (11%).
Patient financial experience
Most respondents (65%) expected local, state and federal regulation of hospital business practices to increase regardless of whether hospitals and health systems improve their business practices related to the patient financial experience (PFE). A smaller share of respondents (21%) said they thought adoption of consumerism-centered business practices at the organizational level may make additional regulation less likely.
Respondents said their organizations have a range of stances on extraordinary collection actions (ECAs):
- 51% haven’t used any since before 2021 and don’t have existing ECA policies
- 15% use ECAs and haven’t made any policy changes on it since 2021
- 15% have modified their ECA policies since 2021
- 13% have ECA policies but haven’t used them since at least 2021
- 6% have discontinued ECA use
Survey respondents were most likely to “somewhat agree” that their patients would give them five stars for their overall financial interactions with the organization.
So far, AI appears to have had a limited role in improving patient financial interactions:
- 51% said it is too early to predict the impact of AI on the patient financial experience
- 21% expected AI to improve the PFE
- 20% expected AI to provide essential efficiency for the PFE





