Staffing issues fuel healthcare unionization efforts nationwide
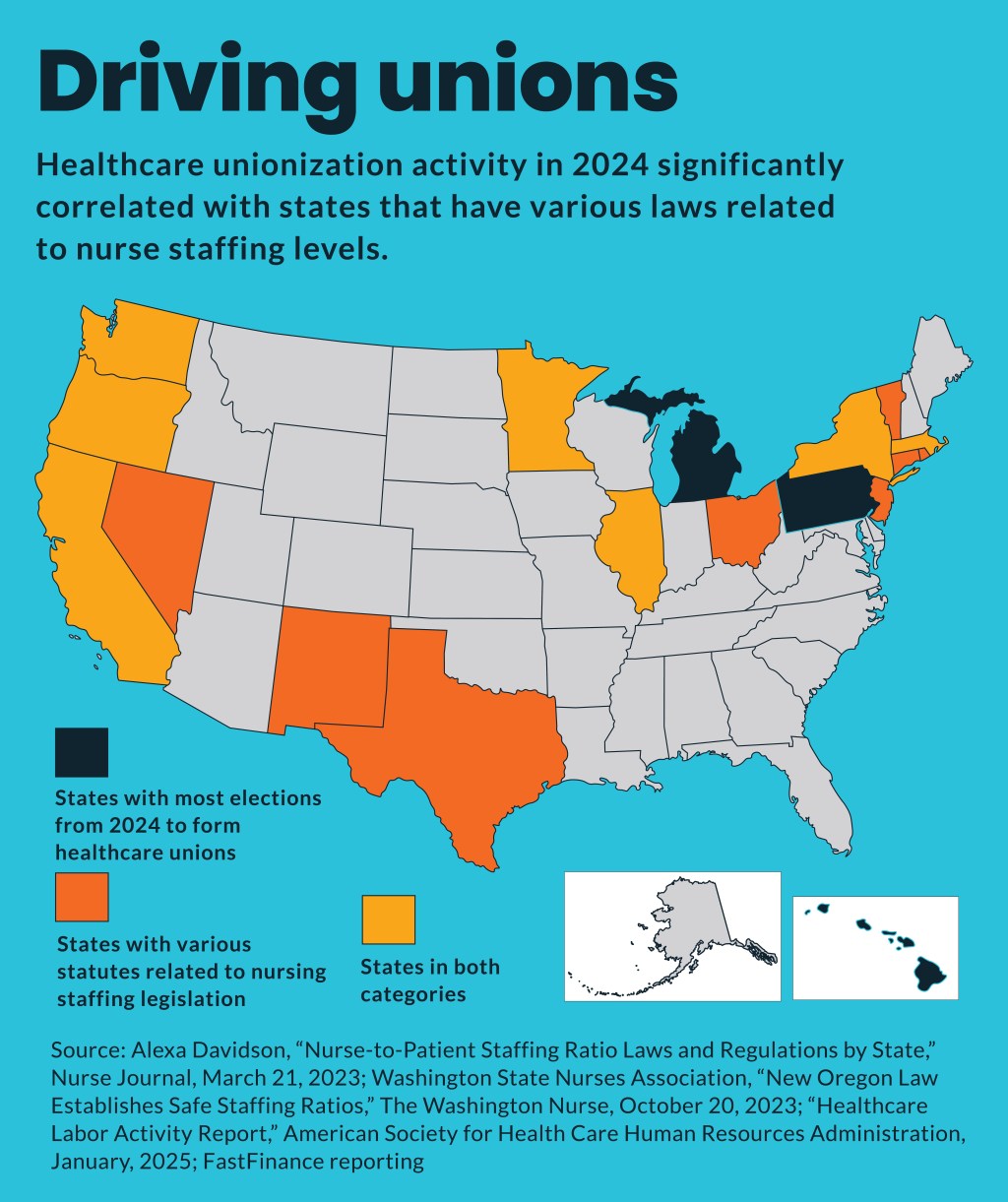
The recent surge in union-forming activity correlates with states that have mandated nursing ratios.
The inability of hospitals and health systems to refocus on employee satisfaction post-pandemic is fueling a continuing increase in healthcare unionization, say those who track the issue.
Healthcare union elections and union wins both increased in 2024, according to the latest labor report from the American Society for Health Care Human Resources Administration (ASHHRA).
The report found 356 healthcare elections in 2024, or 21% more than in 2023.
The trend comes amid a strike by 31,000 workers at Kaiser Permanente. Although most union formation efforts and strikes highlight demands for increased pay, both are fundamentally driven [by] employees believing they are mistreated, said Joe Brock, president of Reliant Labor Consultants and a hospital labor relations adviser.
“Hospitals that fail to keep up with treating their employees with respect, they get unions,” said Brock, who was a former Teamsters president.
The labor and workplace disruptions that occurred during the COVID-19 pandemic initially drove such employee anger, when hospitals focused on operational responses to the detriment of employee morale.
“Ever since COVID, they had those issues, obviously, and hospitals struggled and never really have recovered from that,” Brock said.
Emerging complaints
New issues have arisen that have further fueled employee discontent.
Changes include a shifted workforce with new expectations. That stemmed from the so-called great resignation of boomer-age nurses and others and their replacement by younger staff. Replacement staffers put a premium on schedule flexibility and control over working hours.
“In the past, it was more understood, ‘You will work this many weekends, that’s what the shifts are,’” said Pam Damsky, a managing partner for Chartis. “Some of the younger generation don’t want to do that and only want to work the shifts they want.”
A second challenge is that the wave of departures also hit management ranks, Damsky said. That has left many more supervisors less experienced in addressing employees’ expectations.
“In some roles it’s gotten harder because you’ve got all inexperienced staff and that just makes it harder on everybody, including the more junior staff,” Damsky said.
A third challenge for hospitals is that some organizations have made more progress in addressing employee satisfaction. When staff hear about such initiatives and tools at other hospitals, it can fuel discontent that their own employer does not offer them, said Damsky.
Where unions are rising
Staffing issues are the most frequent driver of employee discontent.
“A lot of what unions’ organizing activity is around is staffing levels,” Damsky said.
The recent increases in union activity strongly correlate with the 16 states with statutory requirements focused on nurse staffing ratios, which include:
- Mandated nurse staffing committees (nine states)
- Required nurse-to-patient ratios (four states)
- Mandated staff reports (five states)
ASHHRA found that 78% of 2024 healthcare elections occurred in 10 states: California, Hawaii, Illinois, Massachusetts Michigan, Minnesota, New York, Oregon, Pennsylvania and Washington. All but three — Hawaii, Michigan and Pennsylvania — were among those with one of the three statutory requirements around nurse staffing.
“For unions in healthcare, their old standby is staffing ratios,” Brock said. “They will always fall on the sword of ‘We can make them staff appropriately,’ and they never or rarely come through” on that.
Despite the correlation to state staffing laws, hospitals nationwide believe they face some unionization risk.
“Some [hospitals] are going to be more sensitive to it than others based on the organizing activity in the state and what they are hearing from their state or neighboring states,” Damsky said. “But I have clients with phenomenal [employee] scores, who are still always keeping an eye out for that.”
Staff responses
Some organizations have found effective responses to the employee unrest that feeds unionization, said Damsky.
“People join unions when they are unhappy with management,” Damsky said.
Effective counter-unionization strategies include:
- Recognizing employee value, cutting unnecessary tasks, using top capabilities
- Ensuring the organization is committed to them, personally and professionally
- Creating an infrastructure to ensure accountability for those priorities
“When those are not in place, you have friction, you have burnout, you have higher turnover rates, and in some cases, you have [union] organizing activity,” Damsky said.
Countering unionization
Brock said hospitals facing a union organizing push need to focus on educating their employees.
First, the union replaces a direct relationship between employees and the organization with a relationship between the union and the hospital, he said.
Employers should educate employees on relevant federal laws, the collective bargaining process and that there is potential for them not to gain anything or even lose something they value after unionization, he said.
Union organizers “make it emotional because if people make a business decision and they go by facts and figures and wages and benefits, and they learn about how it works, it ends up not being a good issue” for workers, Brock said.
One irony of unionization is that contracts frequently require nurses to work overtime hours in order to ensure staffing ratios, which are sought by unions, are maintained when other staff become unavailable. And many union members focused on scheduling constraints are upset when they discover that.
“When you mandate staffing ratios and four people call out sick on the next shift, you have no choice but to keep people,” Brock said. “So, it’s a double-edged sword.”
Other trends
Newer unionization trends include an increasing number of resident physicians forming them. A high-profile example was the first unionized contract for resident physicians at Massachusetts General Hospital that were signed in May.
The nursing staff driving unionization initiatives Brock has examined frequently staff emergency departments.
“Hospitals sometimes don’t provide enough security or safety for those employees,” Brock said. “So, they join a union because the union will promise them that safety.”
Despite a surge in administrative staff in recent decades, Brock said he rarely comes across unionization efforts by back-office staff. Administrative staff most likely to unionize are low-level clerical staff, like cafeteria workers.





