Private equity ownership boosts hospital profitability through staff cuts
The study examined on 281 deals, involving 610 hospitals, where the acquirer was a either a PE firm or a non-PE for-profit organization.
A key to superior financial results and survival of private equity (PE)-acquired hospitals is long-term reductions in non-clinical staff, according to new research.
The study in the September issue of the Journal of Financial Economics also found unchanged clinical outcomes for certain conditions but other researchers challenged their clinical findings.
The study’s financial results for PE-acquired hospitals, from 2001 to 2018, included:
- Better survival rate of PE-acquired hospitals, compared to non-PE for-profit acquisitions
- 7% decrease in wage costs over four years post-acquisition
- 9% cumulative wage cost decrease in fifth to eighth year post-acquisition
- Decrease in total employee-to-patient ratio acquisition
- Increased profitability
- 10% reduction in patient volumes
- No significant change in case mix index (increases can indicate upcoding)
- 1 percentage point decrease in the proportion of Medicaid and Medicare patients
“Importantly, we note that PE target hospitals do not generate significantly higher revenue, which suggests that the increased profitability … likely arises from reduced costs,” wrote the authors.
Compared to non-acquired, matched control hospitals during the study period, PE-acquired hospitals were:
- Significantly more profitable
- Increased operating income and return on assets each by 4 percentage points in the first four years after the acquisition
“Contrary to the concerns raised in the popular press that PE firms tend to close hospitals, we find no evidence of excessive closure [more than non-PE for-profit acquisitions] of PE-acquired hospitals,” the study authors wrote. “PE-acquired hospitals significantly improve their operating profitability, although this effect becomes statistically insignificant in the long-run.”
Labor difference
Labor findings for PE-acquired hospitals included:
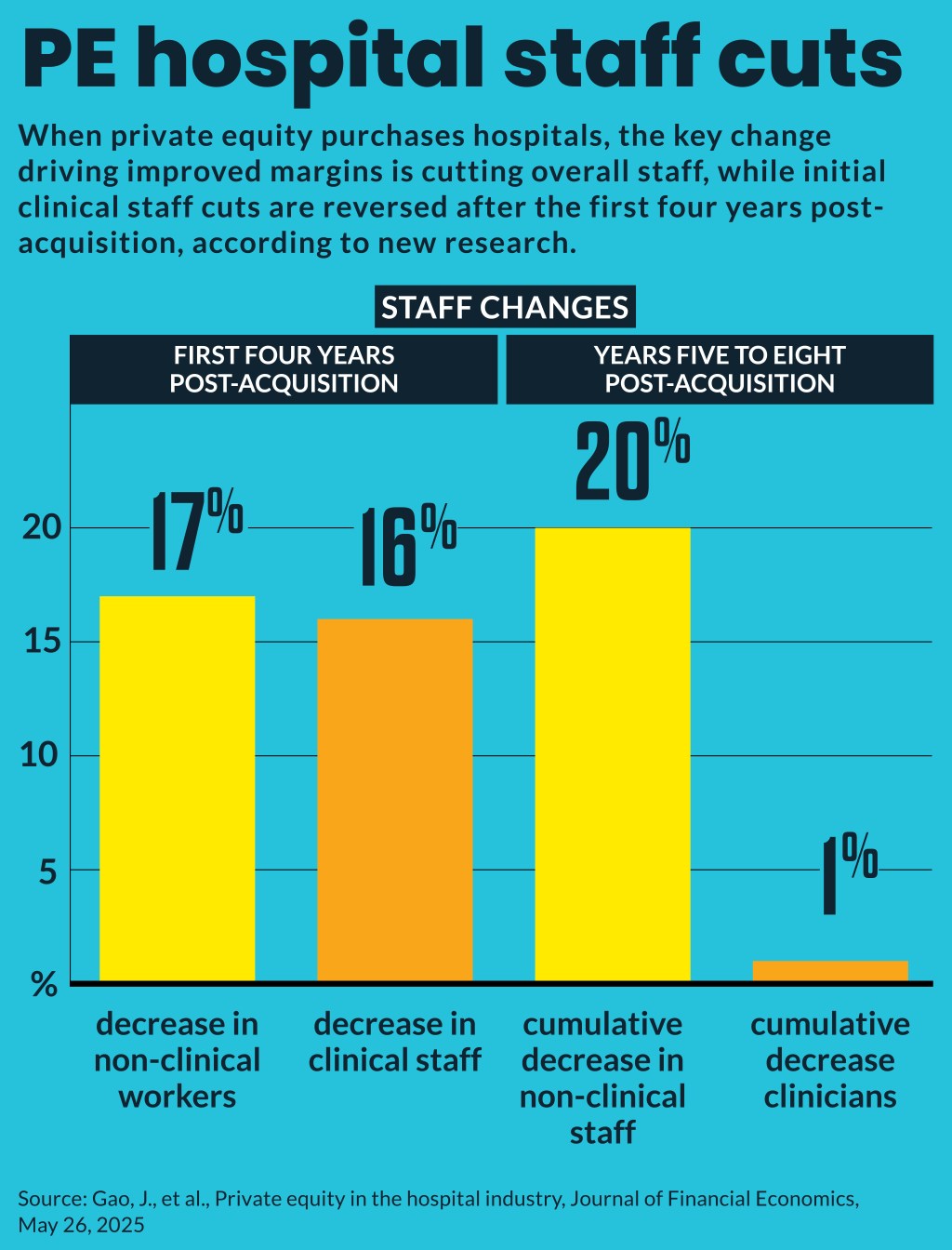
- 17% decrease in non-clinical workers in first four years post-acquisition
- 20% cumulative decrease in non-clinical staff in years five to eight post-acquisition
- 16% decrease in clinical staff in first four years post-acquisition
- 1% cumulative decrease in clinicians in fifth to eighth year post-acquisition
- Deeper workforce cuts if acquired hospital was not-for-profit rather than for-profit
“From what we see, this cost is not just blindly cut; they don’t cut expenses across the board,” said Janet Gao, PhD, lead author and a professor at the McDonough School of Business at Georgetown University. “They cut more of these overhead administrative workers inside a hospital.”
She said the initial decline in clinicians, such as physicians, nurses and pharmacists, probably stems from initial restructuring. And within a few years those clinical numbers bounce back.
“This suggests this type of cost cutting is targeted,” Gao said in an interview.
In contrast, hospitals acquired by for-profit non-PE entities cut clinical staff by 29% in the first four years and another 7% in the next four years. But they did not cut non-clinical workers in either time frame.
The different approaches to labor may indicate non-PE for-profit operators lack the operating expertise, financial engineering capability or governance discipline of PE acquirers, the study concluded.
“There’s a lot of controversy regarding the role of private equity. Some people think it’s absolutely evil because they are going to come into the hospital and sell all of the assets and close down the hospital,” Gao said. “On the other hand, proponents argue they help address the inefficiencies inside the hospital, while keeping the quality of healthcare unchanged.”
The study’s findings were more in line with positive effects PE can have on hospitals, she said.
Cost of administrative cuts
One price for reducing non-clinical staff may have been decreased patient satisfaction.
The study found patient satisfaction decreased across many dimensions at PE-acquired hospitals compared to control hospitals. Similarly, it decreased at hospitals acquired by non-PE for-profit entities.
Although the study concluded the dissatisfaction likely stemmed from service interruptions following the takeover, Gao said it could also come from less administrative services — such as cleaning — that patients may value.
Clinical effects
Gao acknowledged that her study’s clinical data source was “not great” because it provided on three-year hospital-wide rolling averages. Her study found no evidence of increased patient mortality or readmission rates at PE-acquired hospitals.
Zirui Song, MD, PhD, an associate professor of healthcare policy and medicine at Harvard Medical School, who has authored research on PE hospitals, was critical of the study’s examination of mortality data only in commercially insured patients averaging 35 to 44 years old.
“Of course, younger people are much less likely to get these conditions and even less likely to die from them, so it is not surprising they find no changes,” Song said in an email. “They do not study what happens to older or sicker patients, such as Medicare patients, many of whom are dually eligible for Medicaid and particularly vulnerable.”
Song co-authored a study that found PE acquisition was associated with increased hospital-acquired adverse events, including falls and central line–associated bloodstream infections, along with a larger but less statistically precise increase in surgical site infections.
Adrian Diaz, MD, MPH, a fellow in complex general surgical oncology in the department of surgery at the University of Chicago, also noted the study also may have missed adverse surgical outcomes at PE-acquired hospitals.
He co-authored a study published in May that found PE acquisition was associated with a 2.7-percentage-point increase in 30-day postoperative mortality compared with control hospitals.
“When we use patient-level data that’s not aggregated, it’s more granular; methodologically you’re able to pick up some subtle nuances, some subtle shocks that might happen in a short window of time that might be lost otherwise when you aggregate at the hospital level,” Diaz said in an interview.
More research is needed to better identify shortcomings in PE-run healthcare, said Diaz.
“Private equity is here to stay in healthcare, so rather than fighting it and labeling it as all good or all bad, it’s important that we understand the nuances of where and how it would be beneficial and where its limitations lie so we have less blind spots for it,” Diaz said.





