Soaring charity care grabs hospital leaders’ attention
As uncompensated care mounts, experts cite a high rate of denials among factors driving the trend.

Across the country, hospitals are reexamining their approach to uncompensated care, with first movers in this space increasing the availability of financial assistance and working harder to reduce the chances that an account will be sent to collections.
And now, new data paints a picture of the collective impact of these efforts and other trends that are powering a significant uptick in charity care and more accounts being written off as bad debt.
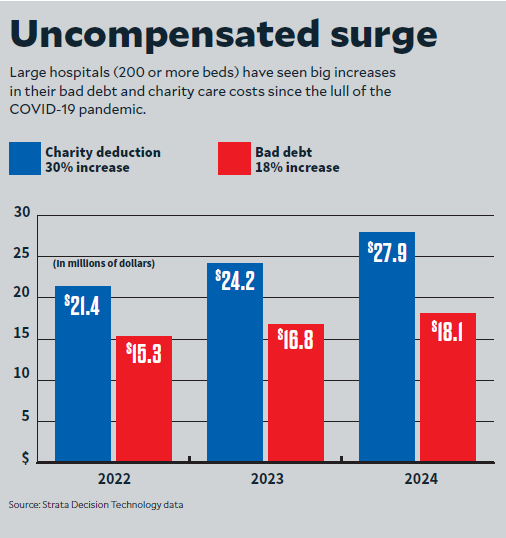
Full-year charity care deductions for hospitals with more than 200 beds surged more than 30% from 2022 to 2024, according to Strata Decision Technology data published in HFMA’s FastFinance newsletter.a Meanwhile, bad debt rose 18% during the same period.
The increase came even as hospitals waited longer to write off medical debt.
“One thing we’ve seen since the course of the pandemic is that the duration of days before hospitals are writing off that debt has grown,” said Erik Swanson, managing director, Kaufman Hall, which uses Strata data for monthly analyses on hospital performance. “So I think they are continuing to pursue — or aim to collect — on those accounts to a longer degree than they have in the past.”
That has led to an increase in overall days in accounts receivable, he said.
Behind the data
Swanson noted that the rise in charity care as well as bad debt is fueled in part by higher rates of denials, an uptick in emergency department (ED) visits from uninsured and underinsured patients, and larger volumes of higher-acuity hospital patients.
Gerry Brogan, MD, FACEP, senior vice president and chief revenue officer at Northwell Health in New Hyde Park, N.Y, has witnessed the impact of these trends firsthand.

“One of the things we understood, because we work with patients so closely, is that most patients don’t show up to the emergency department with all of the required paperwork to apply for Medicaid when all of a sudden they have a car accident,” Brogan said. “People don’t generally carry these forms with them.”
But there are other factors at play as well, experts say — and together they are reshaping hospitals’ approach to charity care and financial assistance.
“Top-performing organizations are figuring out ways to do this with an empathetic approach,” Swanson said.
4 trends giving charity care a makeover
Here are four trends fueling the new landscape for charity care — and early lessons learned from hospitals that are reimagining their approach.
1) It’s easier than ever to estimate affordability for the patient.
The availability of predictive tools for determining propensity to pay has prompted many organizations to revamp charity care eligibility processes. Some automatically run presumptive eligibility checks, notifying patients of positive determinations afterward.

“The availability of risk-scoring models or propensity-to-pay tools creates two downstream effects,” Swanson said. “On the charity side, it’s helping hospitals do a better job of determining whether someone is eligible for charity care. It also helps identify patients who might qualify for insurance coverage they are not yet enrolled in, like Medicaid or CHIP [the Children’s Health Insurance Program].
“On the bad-debt side, revenue cycle teams are using propensity-to-pay tools on the back end to organize work queues according to the likelihood that hospitals will be able to collect the out-of-pocket amount due,” Swanson said. “This enables revenue cycle departments to more quickly write off accounts that are likely uncollectible as bad debt.”
One South Dakota health system, Monument Health, based in Rapid City, collaborated with its collection agency for more than a year to design a formula for presumptive eligibility. Since the model was implemented in August 2023, more than 4,200 people have received financial assistance.
Among patients, “It creates trust that probably wasn’t there before,” said Monument Health CFO Austin Willuweit, FHFMA, CPA, MPA.
Monument Health has heard from both health systems and collection agencies that have expressed interest in learning more about the health system’s success around presumptive eligibility.
“We tell them, ‘Don’t be afraid to make a move like this,’” Willuweit said. “You kind of need to change your mindset and get over the hump a little bit. There will be instances where you granted charity care and left a small amount of money on the table, but over time, you’ll see the greater good you’re achieving for your communities and the patients you support.”

Make sure to notify patients regarding presumptive eligibility determinations.
“You’d think that [notifying patients of presumptive eligibility determinations] would happen normally, but there is a category of financial assistance that is granted on a presumptive basis,” said Keith Hearle, founder and president, Verité Healthcare Consulting. “When this happens, patients might never know they qualified for and received assistance unless the hospital makes communication of this decision part of its process.”
2) It’s expensive to collect from patients.
As the proportion of out-of-pocket healthcare expenses rises — with consumers shouldering on average more than $1,100 in these costs annually — hospitals must decide whether collections are worth the expense.
Hospitals are getting more sophisticated in how they make that decision. Leading organizations are conducting sensitivity analyses to determine the ROI of increasing charity care levels beyond the required thresholds.
“They’re doing the math to determine the point at which increasing total charity care spending as a percentage of gross revenue can reduce the cost to collect on some accounts,” Swanson said.

Consider how your organization communicates availability of financial assistance.
“Educating people up front and guiding them through their financial pathways for care as much as their clinical pathways is essential in today’s world,” said Jason Wolf, president and CEO of The Beryl Institute in Nashville, Tenn.

For example, given that a high degree of charity care provision and bad-debt write-offs stem from care delivered in the ED, Swanson recommends hospitals focus more intently on screening emergency care patients for financial assistance. This might include using digital tools to check for presumptive eligibility and having patient navigators assist patients in completing required paperwork.
“Hospitals must focus on helping patients address their financial obligations more holistically, from helping to obtain coverage to payment arrangements to financial assistance,” said Richard L. Gundling, FHFMA, CPA, senior vice president, healthcare financial practices, HFMA.
3) Healthcare leaders strongly desire to avoid negative consumer sentiment.
There’s an increased understanding of the far-reaching implications of a healthcare organization’s actions around billing and collections, Wolf said.
That’s especially true, he noted, when these actions involve people with limited financial resources or those for whom a life-changing illness or sudden injury has left them in a vulnerable position.
In this environment, Verité’s Hearle is seeing a move away from extraordinary collection actions (ECAs). These include selling the debt to a commercial debt buyer, suing the individual for the amount owed, garnishing wages, denying nonemergency care to people who have outstanding medical debt, or seeking to place a lien on their property.
The best revenue cycle executives also are tightly focused on maintaining goodwill in the community even as they seek to protect their bottom line.
“These leaders are more likely to run successful campaigns in which they ultimately collect on some of what they expect to receive,” Swanson said.

Make sure the hospital’s patient financial assistance and charity care policies match the values of the communities that it serves.
Northwell Health in New Hyde Park, N.Y., for example, allows patients to apply for financial assistance at any point before payment for a service is completed, within 240 days of receiving the first bill.
Brogan said that Northwell has gone so far as to dispatch patient financial services personnel to patients’ homes to help them complete forms to enroll in government health coverage, when needed.
This past May, Cleveland Clinic announced it would require copays beginning in June for nonemergency outpatient services, including scheduled office visits, diagnostic tests and procedures. Those who were unable to make a copayment at the time of service would have their visit rescheduled, the health system stated.b
Later in May, the health system revamped its policy, opting instead for an approach that would be more accommodating to patients who could not afford the time-of-service copayments. While copays for nonemergency services are still required, the health system will allow patients who are unable to make a payment to set up a 0% interest payment plan. The new Cleveland Clinic policy does not apply to Medicaid or Medicare patients. A spokeswoman for Cleveland Clinic declined to comment. However, she did provide a press release, which states that in 2024, more than half of copays due to the health system went unpaid.c
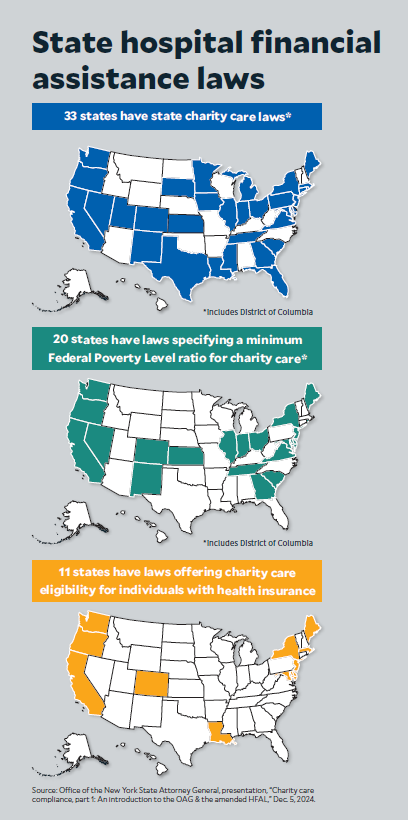
4) States are beginning to make bold moves around charity care — and some hospitals are proactively adjusting their approach.
This year, Oregon became the first state to set spending floors for charity care for not-for-profit hospitals.
The state also expanded hospital financial assistance requirements and created new medical debt protections for patients, such as required screenings for presumptive eligibility when patients owe $500 or more after insurance.
Illinois now requires specific populations to be screened for presumptive eligibility.
And in New York, the state’s patient financial aid law requires hospitals to offer financial assistance to patients with incomes up to 400% of the federal poverty level.d Northwell Health worked with the New York state attorney general’s office to develop best practices for hospital financial assistance and medical debt. The practices included establishing a medical debt ombudsperson whose role is to ensure patients’ ability to pay for care has been taken into account before the health system initiates collection activity.

Invest in tools for presumptive eligibility screening and adopt policies to apply them more broadly, including before care is delivered.
Oregon is currently a leader in presumptive eligibility screening. “To the best of my research, we’re the only state that broadly and blanketly prescreens effectively everybody,” said Steven Ranzoni, hospital policy adviser for the Oregon Health Authority.
And it’s likely that other states will follow suit.
“In 2024, we worked with over 27,000 uninsured patients, and we were able to get 94% of them to convert to some government-sponsored plan that provides them with healthcare,” Brogan said. “When you ask what stands out in my mind, this, to me, is the most important thing.”
These efforts not only help patients pay for the visit at hand but also support access to care for the long term — “maybe for the rest of their lives,” Brogan said.
“This is probably, in my role as chief revenue officer, the thing I’m most proud of that we do here,” he said. “We help improve access to care.”
Determining the right path forward
As the charity care landscape continues to evolve, one thing is clear: Educating patients on options for financial assistance at multiple points in the care journey will be crucial.
It’s an area where Brogan believes hospitals could make a greater impact by working together so that they can learn from one another.
“From our work with the attorney general’s office, I think what we learned is the degree of variability that exists across the state [around financial counseling and assistance],” he said. “Sharing best practices would probably be very helpful in connecting with those who may not be seeking care because of a concern around inability to pay.”
The impact of such efforts would be felt by the communities hospitals serve.
“There’s a huge opportunity to be really intentional about how you’re communicating financial assistance options,” Wolf said. “We really need to advocate for systems that clarify the financial burdens of healthcare and make that transparent to consumers so that the pathways are clear — and that can’t just be an institution-by-institution thing. It should be a collective effort among health systems to get this right.”
Footnotes
a. Daly, R., “Bad debt, charity up 32% since 2022,” FastFinance, HFMA, May 13, 2025.
b. Kosich, J., “Cleveland Clinic to require payment of copays before outpatient visits or appointments will be rescheduled,” News 5 Cleveland, May 13, 2025.
c. Cleveland Clinic, “Update on Collection of Copays,” May 28, 2025.
d. New York State Department of Health, “Hospital Financial Assistance Programs for Patients,” revised February 2025.






